- We want to see your poop.
- You’re getting an IV.
- Take a class or a tour.
- Your first labor & delivery is the longest.
- Get a doula.
- Let go of control.
- It’s only one day.
- Are you with the right doctor?
- Say something.
- How to thank us.
We want to see your poop.
Let’s get this one out of the way first because it’s my favorite. Everyone who comes into L&D to have a baby is worried about “pooping on the table.” They think that they are going to try and push a baby out, and the baby will stay inside their body, and instead a huge poop will come out and it will be mortifying. Wrong!
When you are completely dilated (10cm) the only thing holding your baby in is your pubic bone. Pushing is the act of bearing down to rock baby under your pubic bone and stretch/make space for your baby in your vagina. When you are doing a great job of pushing, if (big IF!) there happens to be stool (medical term for poop) in your rectum (medical term for butt) at that time (and maybe there isn’t because diarrhea sometimes happens in earlier labor), a little smear of poop might come out with pushing.
Nurses think this is a great sign that you are pushing effectively! We like to see this! We are usually quite good at keeping this discrete. I keep a “poop drape” towel tucked under your bottom and folded up to hide your bum. We change these towels often, and chances are you will have no idea if there was a little bit of poop or not. Ditto for any support people in the room at the time.
You’re getting an IV.
Please don’t write a birth plan that says “No IV unless medically necessary.” You’re all getting IV’s. Think of an IV like buckling your seatbelt when you get in a car. It’s for safety. It’s for just in case. There are people who say “telling moms they need IVs in case of emergency is hospital fear language and negative because it implies there may be emergencies.”
There are people who say “can’t you just start an IV if there’s an emergency?” These people have obviously never started an IV and have never been in a true medical emergency. It’s not always easy or quick to start IVs, so we like to place them soon after arrival to the hospital. An IV is a tiny plastic straw inside a blood vessel. The needle we use to get that straw under your skin doesn’t stay in! Lots of people fear IVs because they mistakenly believe a needle is going to stay inside them. Wrong, it comes right out immediately!

The straw (catheter) is connected to a small access port. We can connect that access port to a longer strand of tubing and use it to infuse fluids or medications. If the straw and port are not connected to the tubing, it’s called a “saline lock” or a “hep lock.” But the IV part remains the same. Please don’t write a birth plan that says you want a “saline lock instead of an IV.” That doesn’t make any sense. If you don’t need to be connected to fluid or medications, we will disconnect the long tubing so you will have more freedom of movement.
If you don’t think you need extra fluids and you aren’t requiring medication at the time, it’s always ok to ask for your IV to be saline locked. Requiring patients to have IV’s isn’t a thing that’s going to change anytime soon in the hospital setting. If this is really a big deal for you, look into giving birth at a birthing center or at home.
Take a class or a tour.
If you took a childbirth preparation class, you would have already heard that pooping pep talk, and heard that you’re getting and IV, and had the chance to ask a birth professional anything you wanted! Classes are amazing for lessening anxiety and fears, building confidence, empowering you to make informed decisions about your health care, even teaching you the anatomy basics. I started teaching classes because I couldn’t believe how many times I would be holding a woman’s dilating cervix in my fingers talking to her, and she had no idea what that was or its very important role in labor. Get informed!
At the very least, take the tour of the hospital’s birthing facilities. It’s packed with information, tips, and you get to ask the nurse leading the tour any and all questions about policy or procedure.
Your first delivery is the longest.
Your first labor and delivery usually takes the longest time of any pregnancy you will have. Be patient. Be more patient than you ever thought possible. It can take days or weeks for your cervix to soften, efface and start to dilate. Then it takes awhile to dilate to 4cm (awhile = hours or days). Then it takes about a centimeter an hour to go from 4cm to 10cm. And then it takes anywhere from 20 minutes to one, two, or three hours to push your baby out.
While we’re on the topic of things you should know: know that your doctor won’t come push with you until the very end, like the last several pushes. You could push with your nurse for two hours, and the doctor two pushes. Might as well tell you all of it: it might not even be your doctor. It might be one of your doctor’s partners.
The active labor portion of this whole experience (where contractions are strong and require all your coping attention) can start at any time of the day or night, so maybe you end up being awake for a long time. Even if you are planning on having an epidural, you must come prepared to cope with strong contractions. We will help you cope of course, but it’s naive to think it’s possible to feel nothing.

Many of the epidurals I help administer to patients are for exhaustion, not inability to handle pain. We call it “therapeutic rest” and is very common for first time moms.
Coincidentally, the time when most women think they want to try and have a baby without an epidural is the first time they are pregnant. It’s like if someone tried running for the first time and found out the course was a marathon. Some people might reasonably decide, well running isn’t for me. I sure would. The problem with this is that the second meeting of the running club is just a 3 mile loop around your neighborhood. Your second, third etc labors are much faster! Like, hours and hours faster! Once strong labor contractions start your cervix can dilate to 10cm very fast.
We joke that we don’t trust those moms for a minute. They could “go complete” (-ly dilated) at anytime and push that baby out in minutes. My point is, don’t beat yourself up if you thought about not getting an epidural with your first delivery and you ended up having one. Maybe try it with your next delivery, or…
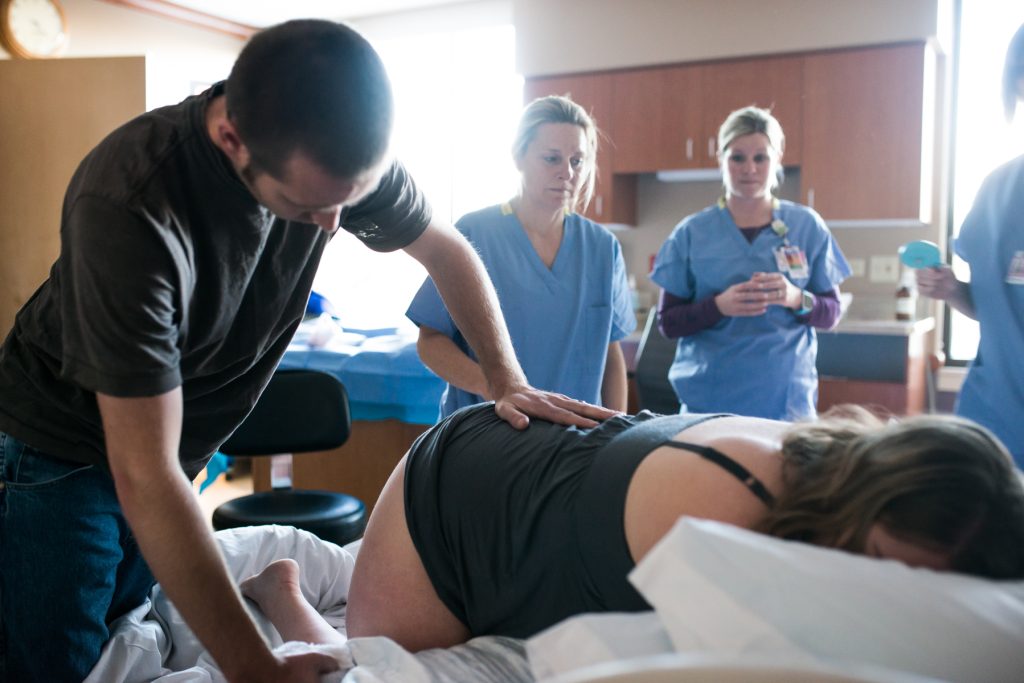
Get a doula!
If you are a first time mom and your goal is to deliver epidural free in a hospital setting, think about getting a doula. When you are in the hospital, a doula and I aim to do basically the same thing for you, with one catch. The doula only has to do it for you. Sad but true, I may have another patient I am taking care of at the same time as you in the early part of your labors. Additionally, your doula usually starts caring for you at home in early labor. This can keep you home for a longer amount of time than if you were laboring alone.
Constant, reassuring, expert bedside support is crucial for managing natural labor. Doulas can be expensive. If you can’t afford one, make sure that when you first arrive as a patient in Labor & Delivery, you ask to speak to the charge nurse and request a nurse who loves working with natural labor patients (we all are capable of doing this, some just have a special passion for it).

Let go of control.
There is a huge spectrum of normal in Labor & Delivery, and you can’t plan it all out in advance. You just can’t. Trust your support team and your providers to give you good advice and expertise, ask the right questions, and pay attention to your intuition. Breathe. Think of this as your initiation into parenthood. Anyone who’s been around kids knows “control” is not a word used to describe the experience of raising young children. More like: “SURRENDER”, “LET GO”, “WHAT WILL BE WILL BE”, “BE OPEN TO THE EXPERIENCE”, “RIDE THE WAVE.” Coincidentally those are great birth mantras. Another one of my favorites: “Let go or be dragged.” Breathe. It will be ok.
This is only one day.
Ok, maybe it’s two or three or four days, but your time being in labor and delivering a baby is relatively short. It can be an empowering, life changing, positive experience, but it is still only several days. Parents spend so much time preparing for (and worrying about) this portion of the experience (where you will have a constant bedside presence of a supportive L&D nurse or doula), and neglect preparing for the postpartum period (where you will be sleep deprived at home with another sleep deprived person as your companion and a confusing tiny new member of the family who you love in a terrifying way).
Labor is one experience. After your baby is born, breastfeeding is an experience that is going to happen every three hours for almost the next three months or longer. Breastfeeding is natural, but it doesn’t come naturally. Babies and moms have to learn those behaviors. Take a breastfeeding class; identify three friends who have breastfed successfully that you can text with questions; and get the name of a good lactation consultant in town. Most breastfeeding issues come up after you’ve been discharged from the hospital. Not breastfeeding? No judgment here, fed is best.

Make a postpartum care plan (great book). Put just as much effort into that care plan as your list of birth preferences. Identify a new moms group you can go to, an online community, or a postpartum doula service to come love on you at your house if needed. Make a plan for postpartum mom not being the person solely responsible for dealing with household chores, cleaning, cooking, laundry, etc. Make a plan to have friends drop off dinner. Key words: drop off. You’re not hosting people to dinner every night. Drop off food and leave, thanks. People who understand this are the best kind of people to include in your postpartum plans.
Be kind to yourself. Let your house be a mess. Just a total mess. The default position is on the couch with a baby skin to skin, feeding when needed, next episode on Netflix starting in 12 seconds. Be kind to your postpartum body. Don’t say mean things to it or think mean things about it. It’s beautiful. You’re beautiful. You just did a beautiful thing.
Postpartum depression is real. Postpartum anxiety is real. Weepy is normal. Feeling hormonal and overwhelmed is normal. It’s ok to feel like you should be so happy but you’re just not. If this lasts longer than three weeks or you have thoughts about harming yourself or baby call your doctor or midwife immediately and get an appointment to see them in person. If you feel traumatized by your birth experience, talk to someone. Partners and friends can help, but don’t be shy to talk with your providers. And ideally, if you were delivered by a different provider in that practice, make your follow up postpartum appointment with them. Maybe they can help you work through and process some decisions and emotions from that day. You’re not alone. Seek out postpartum mental health support group or alliances in your town.

Some of you are with the wrong doctor.
We scratch our heads over this one all the time. Let’s say Doctor A and her partners are the group at our hospital who have the highest volume of pain med free deliveries (what a lot of people call “natural” childbirth), and the lowest rates of interventions (inductions, C-sections etc). Doctor Z and her partners have the highest rate of epidural deliveries and highest rates of interventions, with all the other practices that deliver with us having A-Z variations in between.
It is always perplexing to us nurses when patients with goals and philosophies similar to Doctor A group (and usually quite adamant about their desires) show up but are patients of Doctor Z group. You’d be better matched with another doctor, but our hands are tied. When we are meeting you, you are already in labor or showing up for an induction. We can’t, and we shouldn’t, tell you then to switch doctors. We can only attempt to navigate you through the maze of possible interventions. This is a finely honed art of professional relationships between the doctor and the nurse.
Our job is to advocate for you and your preferences. Your job is to do your homework. Don’t just choose a doctor because they are popular or your friends go to them or they are already your doctor who’s been prescribing your birth control pills and doing Pap smears for a couple years. Spend some time thinking about your birth philosophies and preferences, ask friends about their births and their providers, and know that it’s ok to interview OB’s before choosing a practice.
You’re the consumer. Say something!
If you have a bad experience in a hospital setting, say something. Not to your friends, not to the internet, say something to the hospital administrators themselves. All hospitals call you in the postpartum period for a follow up survey. This is your chance to tell us the things we got right, and what areas we need to improve. Be specific. If you didn’t get this call, or you didn’t realize you could speak so openly during that call, call the hospital back. Ask to speak to the unit manager or director. These days, patient voice and satisfaction is everything in health care. Almost to a frustrating degree, hospitals will listen to what patients say more than what the nurses say. Upset about some of practices you encountered in L&D that you don’t feel are evidence based medicine? Let them know.
Here are some possible suggestions, wink wink: strict restrictions on eating and drinking in labor, nurse to patient ratios in labor, baby remaining skin to skin with you in the first hour of life, enough staff for breastfeeding support.
How to thank us…
We love to eat still-hot Tiff’s Treats cookie delivery and a baker’s dozen Einstein bagels and cream cheese, but we can live off a genuine thank you note for weeks. I still have every one I’ve ever received, and they are among my prized possessions. Oh, but if you’re going for food we also like breakfast tacos, pizza, coffee…
This guest post was written by Maureen Hodges BSN, RNC-OB, LCCE. Maureen has over ten years of Women & Children’s nursing experience. For the past seven years she has been a Labor & Delivery nurse at a very busy hospital in the Austin area. She teaches private, hospital, and online childbirth classes. She has two children, aged 1 and 3, and a husband who knows all her L&D pep talks verbatim from listening to her answer every pregnant woman’s questions at dinner parties, on airplanes, and on the phone in the middle of the night. She has attended the deliveries of everyone in her book club. She could not pick any of their vaginas out in a line up. You can find her online at @empoweredbirthatx or Empowered Birth Austin on Facebook.

No Comments yet!